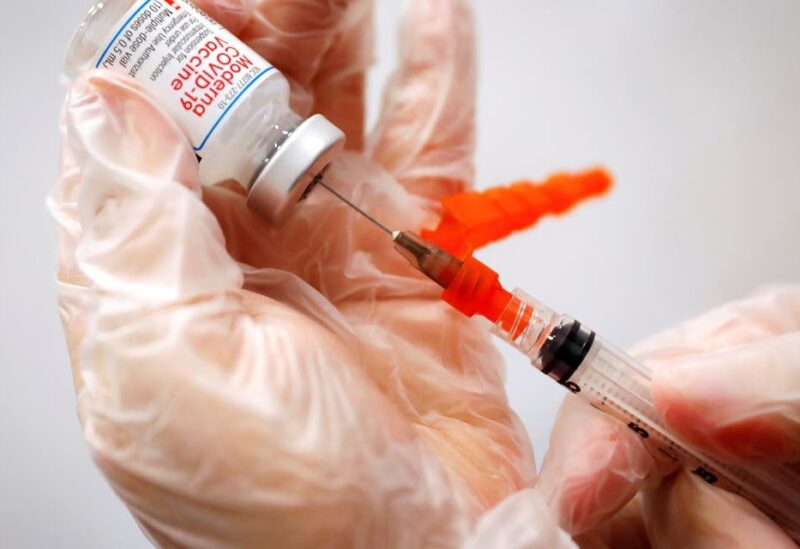
As valid data is used to explain the benefits of getting a COVID-19 vaccine, it is clashing with misinformation and conspiracy theories. At times, building a communication strategy that can direct people to have a jab seems very difficult.
This is made harder when considering that any given population is categorized into three groups: People are either convinced, hesitant, or will reject completely the very thought of taking the vaccine. Let’s be clear; these categories aren’t limited to the people of a single country. It’s a global issue.
Most of the hesitant individuals are the result of the existence of the two other groups: they rest in the middle.
Considering the timeline of the pandemic and the quick drive to vaccine availability, applying incentives work mostly on the hesitant group of society. People in this group do not have their minds fixed on getting the vaccine, nor do they have the complacency of belonging to the anti-vaxxer movement.
This hesitance to have the vaccine comes from a complex spectrum of reasons, and differs completely from the views of anti-vaxxers.
The time the vaccines came to market is an issue; the lack of clear knowledge about which brand is best, and the locations in which they live all play a role.
The lack of understanding of the vaccines has proven to be disconcerting for policy makers who believed public awareness campaigns was making it clear what the vaccines do, why they are being put in place so quickly, and the level of protection they bring.
Worries of unknown complications was also a factor in hesitance, with people unsure about the level of risk to their health when receiving a jab.
Remember, these aren’t the anti-vaxxers. These are ordinary men and women expressing legitimate concerns about the vaccine situation.
These issues have existed since vaccines were first proposed, and then introduced as public health practices. This happened in the early nineteenth century.
Laws that regulated and mandated vaccinations in those early days were opposed by the anti-vaxxers of the time.
Beyond the risks of COVID-19, and the deaths we’ve witnessed, having both the hesitant, and the rejection groups leads to incomplete vaccine coverage, while increases the risk of greater spread of disease for the entire population. This includes for the already vaccinated group. It also decreases the chances of developing herd immunity.
In the past different tactics employed by health authorities to get resistant parents to vaccinate their children had little success. Finally, coercion policies were adopted to ensure vaccination for the welfare of society.
Government health policy makers need to avoid adopting particular forms of incentives. Many are ultimately harmful for society in the long-term. Monetary incentives can easily become a form of coercion, but offering financial rewards to follow good health practices encourages members of the public to expect money for other best health practices.
Incentivizing members of the public to participate in research programs can incorporate consent requirements. If the vaccine receiver in a test group belongs in the hesitant group, and can tell me the expected benefits of the vaccine, then I know he or she comprehends the benefits of being vaccinated. This goes beyond reaching out for the provided incentive.
Incentives are ethically accepted because they fall within the interest of good public health, especially for the role played to contain and mitigate a pandemic. However, a regulating framework is essential in order to maintain the ethical boundaries of encouraging people to take the vaccine.
Considering other ethical principles – such as justice – it might sound unfair to those who already took the vaccine of their own volition, or those that might have been forced to take it.
Vaccine incentives can be viewed as encouraging good behaviour – not in an ideal way, but a compromise is needed every now and then.
A beneficial act that has low risks, regardless if it includes inducement, can be ethically accepted in the name of public health. The justification is that, it is good for the vaccine receiver, their family, their community, and the global community itself, regardless of how small one single person’s inclusion plays.
The WHO considers vaccine hesitancy as one of the top ten global health threats. Thus having regulated incentives is ethical and acceptable because simply put, it is to society’s benefit.