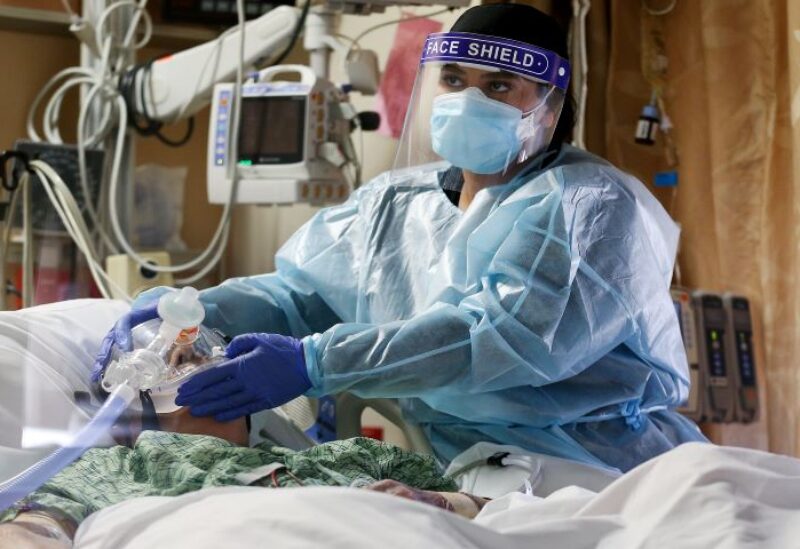
US hospitals
Due to an increase in COVID-19 infections caused by the highly transmissible omicron version of the coronavirus, hospitals throughout the United States are deferring elective procedures to free up personnel and beds.
According to administrators, hospital personnel shortages have been exacerbated in the previous month by medical practitioners isolating or quarantining themselves because they have been sick or exposed to the virus.
A Reuters review of public statements and local media reports found that hospital systems in nearly half of the US states, including Maryland, Virginia, and Ohio, have announced plans to postpone elective surgeries, and at least three state governments, including New York, Illinois, and Massachusetts, have implemented or recommended state-wide delays.
Data from the Centers for Disease Control and Prevention reveal that the majority of locations where hospitals are delaying procedures had a peak or increase in daily COVID-19 hospitalization rates during December or January.
According to Reuters, the omicron spike has also led the National Institutes of Health to postpone elective surgery at the largest hospital in the United States devoted to clinical research.
Suspending elective procedures can generate a backlog of patients, cost hospitals millions of dollars in lost income, and, in some situations, result in serious sickness or death.
Elective care, according to Cynthia Cox, vice president of the Kaiser Family Foundation, can still be critical. During the epidemic, tens of thousands more individuals died from non-COVID reasons than usual, and some of those deaths are thought to be due to delayed care, she added.
“It’s frequently cancer operations or other types of treatment that still need to happen in a very timely manner for people’s safety and health,” Cox explained.
Following a spike in COVID-19 hospitalizations, the Ohio State University Wexner Medical Center, a Columbus-based center with over 2,200 beds across multiple hospitals, is postponing some non-urgent, elective surgeries requiring an overnight stay, according to Dr. Timothy Pawlik, chair of the Department of Surgery and surgeon in chief.
According to the most current CDC data, the seven-day average of daily new hospital admissions in Ohio is at an all-time high.
According to spokesperson Danny Jacobs, Johns Hopkins had to put one of its facilities, the Johns Hopkins Bayview Medical Center, into crisis mode, postponing elective procedures and diverting employees.
According to him, the Baltimore hospital reported a 360 percent spike in COVID-19 hospitalizations in December, the most since the pandemic began.
The Virginia Commonwealth University Medical Center announced the suspension of elective procedures in its downtown Richmond, Virginia, hospital owing to extraordinary demand for inpatient treatment caused by the Omicron variant.
Shy recovery, followed by an omicron hit
According to CDC data, the seven-day average of COVID-19 patients admitted to hospitals increased by 60% from the previous week to 16,458 per day, falling only 0.2 percent short of the national peak in hospital admissions precisely a year ago.
According to data from the US Department of Health and Human Services, over 82 percent of ICU beds nationally were in use as of Thursday, with over 27 percent reserved for COVID-19 cases.
Elective procedures have just recently begun to recover from the delays and cancellations that began when the epidemic struck in March of 2020.
According to a January report, US hospitals lost an estimated $22.3 billion as a result of the cancellations between March and May of 2020.
And now there are even fewer professionals to deal with COVID patients as well as those in need of elective surgery.
According to the US Bureau of Labor Statistics, approximately 450,000 healthcare workers, or 3% of the industry’s workforce, will leave between February 2020 and November 2021.
According to Akin Demehin, director of policy at the American Hospital Association, many institutions are merely delaying certain treatments for shorter periods of time than during the early epidemic.
“From that experience, hospitals have learnt to identify those treatments that really do need to be done as rapidly as possible, and that allows them to be a bit more nuanced in how they could apply deferral or delays,” Demehin added.